Comprehensive analysis of antibody responses could help in the development of a potential vaccine for coronavirus disease 2019 (COVID-19) patients, according to a study published on September 10 in the open-access journal PLOS Pathogens by Chao Wu and Rui Huang of Nanjing University Medical School, and colleagues. The research findings suggest that antibodies’ neutralizing activity from recovered patients is usually not strong enough and declines very quickly within one month after hospital discharge.
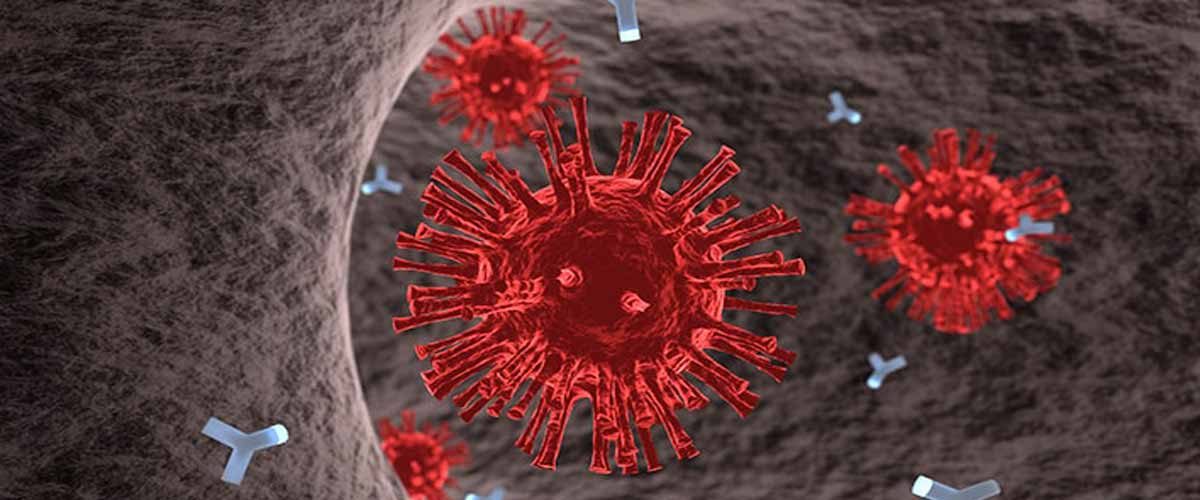
As a consequence of the growing COVID-19 virus, the world faces an unprecedented major challenge with communities and their economic status affected by the pandemic. There is no vaccine or potential drug approved to treat or at least prevent the disease. An improved understanding of antibody responses against SARS-CoV-2 — the virus that causes COVID-19 — will give primary information for preparing effective therapy and a defensive vaccine. In the present study, researchers regularly monitored SARS-CoV-2-specific antibody responses in 19 patients with moderate symptoms and seven severe COVID-19 patients for about seven weeks.
Most of the patients produced antibody responses against SARS-CoV-2, including the viral nucleoprotein and three parts of the spike protein: S1 protein, ectodomain, and the receptor-binding domain. However, 80.7% of recovered COVID-19 patients had unstable antibody neutralization activity against SARS-CoV-2; only a small number of patients obtained an effective level of neutralization activity. This result emphasizes the careful collection of blood samples from recovered patients using antibody neutralization assays earlier to transfusion into other COVID-19 patients. After three to four weeks of hospital discharge, the neutralizing activity of antibodies from recovered patients decreased significantly, signifying that recovered COVID-19 patients might be vulnerable to get an infection with SARS-CoV-2. Furthermore, COVID-19 patients with severe symptoms had a significant amount of non-neutralizing antibodies, contributing to infectivity’s antibody-dependent development. According to the authors, the study provides meaningful insights for antibody-based intervention, vaccine design, and serological trials.
Funding: The Fundamental Research Funds supported this study for the Central Universities (No. 14380459 to CW). The Medical Science and Technology Development Foundation, Nanjing Department of Health (YKK19056 to YC), Nanjing Medical Science and Technique Development Foundation (QRX17141 to YC). The funders had no role in study design, data collection, analysis, decision to publish, or manuscript preparation.











Informative