Seasonal influenza is allegedly no fun, but new findings suggest the colds you’ve had in the past years may give some protection from COVID-19. The research reported by infectious disease specialists at the University of Rochester Medical Center also recommends that immunity against COVID-19 is possible to last a long time — maybe even the entire life.
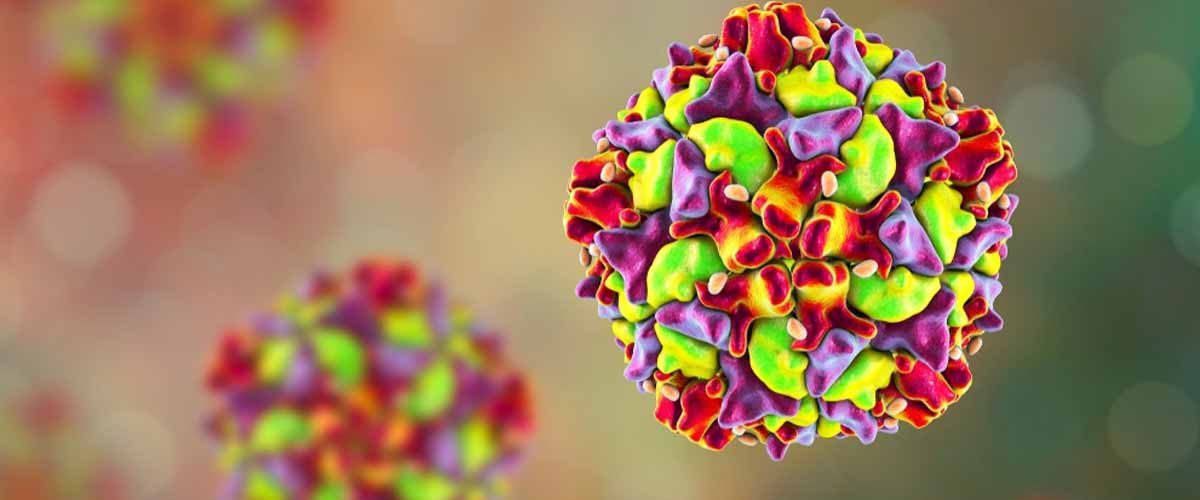
The first study, published in mBio, shows that the virus responsible for COVID-19 disease, SARS-CoV-2, induces memory B cells, long-lived immune cells that identify pathogens, and generates antibodies to destroy them and memorize them for the future. The next time that pathogen tries to penetrate the body, those memory B cells can immediately jump into action to clear the infection before it starts.
Since memory B cells can survive for unpredicted decades, they could prevent and protect COVID-19 survivors from subsequent infections for a more extended period, but further study will have to bear that out.
The research is also the first to report cross-reactivity of memory B cells — meaning B cells that once attacked cold-causing coronaviruses appeared even know SARS-CoV-2. The studies supposes this could mean that anyone who has been infected by a common coronavirus — which is almost everyone — may have some extent of pre-existing immunity to COVID-19.
“When we looked at blood samples from patients who were recovered from COVID-19, it looked like many of them had a pre-existing group of memory B cells that could recognize SARS-CoV-2 and quickly produce antibodies that could attack it,” said lead study author Mark Sangster, Ph.D., a research professor of Microbiology and Immunology at URMC.
Sangster’s results are based on a contrast of blood samples from 26 people recovering from less to moderate COVID-19 and 21 healthy donors whose samples were collected six to 10 years ago — long before they could have been exposed to COVID-19. From those samples, research authors calculated levels of antibodies and memory B cells that target precise parts of the spike protein, which exists in all coronaviruses and is critical for helping the viruses infect cells.
The spike protein looks and works a little diverse in each coronavirus, but one of its components, the S2 subunit, remains pretty much the same across all of the viruses. Memory B cells can’t tell the dissimilarity between the Spike S2 subunits of the different coronaviruses and attack randomly. Estimated, the research found that was true for a subclass and beta coronaviruses that include two cold-causing viruses as well as SARS, MERS, and SARS-CoV-2.
Furthermore, the present study lacks the appropriate information about the extent of the defense provided by cross-reactive memory B cells and how it impacts patient outcomes.
“That’s next,” said David Topham, Ph.D., the Marie Curran Wilson and Joseph Chamberlain Wilson Professor of Microbiology and Immunology at URMC, who runs the lab that conducted this work. “Now we need to see if having this pool of pre-existing memory B cells correlates with milder symptoms and shorter disease course — or if it helps boost the effectiveness of COVID-19 vaccines.”











Great
Very informative however further information on memory B cells will help to develop the appropriate treatment.
Excellent and very useful. Thank you!
Informative!!
Informative study
Interesting
Keep it up.
Great. Useful and valuable information
Very much informative. Didn’t know about memory B cells.. These cells will help to create the appropriate cure for this treatment
In practice most patient exposure to Covid19 have multiple attack flu in the past These against the study
but new findings suggest the colds you’ve had in the past years may give some protection from COVID-19? It means that if any one had a common cold in the last year may protected from COViD-19
I’m not sure why this information hasn’t been exploited months ago. It has been pretty well known that there was some cross reactivity with coronaviruses that cause common cold, at least 4 have been in circulation for decades, and have been isolated in virology laboratories.
This is a good data and give us a hop for future. About immunity of our body and give protection also not fried from future with this new emerging virus
This is a good information to our immune system